Thyroid Resistance Syndrome and Reverse T3
Thyroid Resistance Syndrome (RT3)
Thyroid resistance syndrome occurs when the body converts T4 (Thyroxine) to an inactive form of T3 (liothyronine), known as reverse T3 (RT3). This can happen independently or in individuals taking T4-containing medications like Synthroid or porcine glandular medications such as Armour Thyroid. The conversion to RT3 is influenced by various conditions within the body.
What is Reverse T3 (RT3)?
Reverse T3 is an inactive form of T3. The body has a built-in mechanism to regulate the balance between T3 and RT3. Under certain conditions, this balance can be disrupted, leading to a higher conversion rate of T4 to RT3. This imbalance can be measured by calculating the ratio of Free T3 (FT3) to RT3, with a healthy ratio being greater than 20.
Consequences of Excessive RT3 Production
Excessive RT3 production can lead to significant health issues. RT3 binds to T3 receptor sites, preventing the active T3 from exerting its beneficial effects. This results in a state of functional hypothyroidism, where patients exhibit hypothyroid symptoms despite having normal lab results. Symptoms can include fatigue, weight gain, depression, and other common signs of hypothyroidism. Patients often experience a cycle where they feel better after increasing their medication dose, only for symptoms to return, indicating thyroid resistance syndrome.
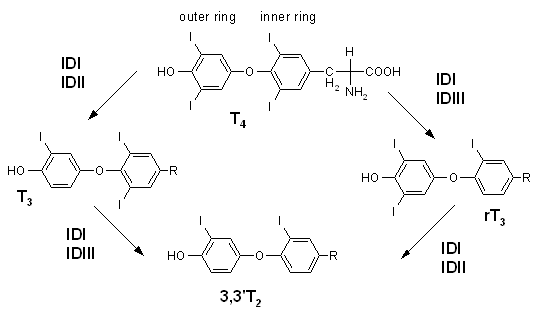
Visual Comparison of T3 and RT3
T3 and RT3 are similar in structure, with the key difference being the position of one iodine molecule, creating a mirror image (isomer) of T3. Despite their similarity, RT3 is completely inactive and blocks the receptors from utilizing circulating T3.
Importance of Recognizing Thyroid Resistance Syndrome
Identifying and addressing thyroid resistance syndrome is crucial for effective management of hypothyroidism. Patients often suffer if this condition is not diagnosed and treated appropriately. Those who experience frequent dosage increases without sustained relief may be particularly affected by this condition.
Further Reading from Top Journals
- Thyroid Hormone Concentrations, Disease, Physical Function, and Mortality in Elderly Men: This study explores the relationship between thyroid hormone levels and various health outcomes in elderly men.
- A Study of the Extrathyroidal Conversion of Thyroxine (T4) to 3,3',5-Triiodothyronine (T3) in Vitro: Investigates the biochemical pathways and factors influencing the conversion of T4 to T3 outside the thyroid gland.
- Small Differences in Thyroid Function May Be Important for Body Mass Index and the Occurrence of Obesity in the Population: Examines how minor variations in thyroid function can impact body weight and obesity prevalence.
- Replacement Therapy for Hypothyroidism with Thyroxine Alone Does Not Ensure Euthyroidism in All Tissues, as Studied in Thyroidectomized Rats: Highlights the limitations of T4 monotherapy in achieving optimal thyroid function across different tissues.
Why Choose Integrative Health Solutions for Thyroid Resistance Syndrome (RT3)?
Integrative Health Solutions and Dr. Bronner Handwerger NMD have been providing cutting-edge thyroid treatment to patients for 20 years. We have become the leading experts in thyroid treatment in San Diego. Here are some of the reasons why you can trust the team at Integrative Health Solutions:
Advanced Technology
At Integrative Health Solutions, we use advanced testing methods to identify underlying issues. We stay ahead by using the most advanced technologies available.
Qualified Professionals
Our leading doctors are experts in the field of endocrinology and thyroid conditions and treatments.
Thorough Approaches
Our solutions and approaches to treatment look at all aspects of health to balance and optimize the patient’s well-being.
